If you have nerve pain from diabetic neuropathy, sciatica, or peripheral nerve damage, you’ve probably tried multiple treatments. Some helped. Many didn’t. But there’s one angle most people skip: what you eat may be directly affecting how bad the pain feels.
Over the past five years, researchers have taken this question seriously. This article analyzes 18 clinical studies published between 2020 and 2025 to answer one thing: can changing your diet actually reduce nerve pain?
What we cover:
- Clinical evidence from 18 peer-reviewed studies
- Effectiveness data by diet type
- Specific anti-inflammatory nutrients that target nerve pain
- Comparison of Mediterranean, plant-based, and low-calorie diets
- Practical steps based on research protocols
Disclaimer: This article synthesizes published medical research for educational purposes only. Consult your healthcare provider before making dietary changes, especially if you have diabetes or other medical conditions.
Understanding the Inflammation-Nerve Pain Link
Inflammation isn’t just a buzzword. It has a direct, documented effect on nerve pain, and the mechanism matters.
The Science Behind Neuroinflammation
When nerves get damaged, the body triggers an inflammatory response. That response produces pro-inflammatory cytokines including TNF-alpha, IL-1 beta, and IL-6. It also releases mediators like prostaglandin, serotonin, and bradykinin. These substances activate and sensitize pain receptors, keeping the pain cycle running long after the original injury.
A 2016 review in the Journal of Ethnopharmacology documented how inflammatory mediators act on nerve tissue through both direct and indirect pathways. The same research noted that some immune cells also produce anti-inflammatory cytokines and opioid peptides like beta-endorphin, which can naturally reduce pain.
The practical implication: diets that reduce systemic inflammation may interrupt the pain cycle by lowering inflammatory mediator production and improving the integrity of the intestinal barrier, which prevents certain metabolites from entering the bloodstream.
Systematic Review: Diet Types and Nerve Pain Outcomes
1. Mediterranean Diet for Diabetic Neuropathy
The Mediterranean diet focuses on olive oil, whole grains, vegetables, legumes, nuts, and fish. It’s the most researched dietary pattern for managing nerve pain linked to diabetes.
Study 1: Spanish Observational Study (2020-2023)
A pilot study of 174 patients with type 2 diabetes, published in the Journal of Endocrinological Investigation (2024), looked at the relationship between Mediterranean diet adherence and diabetic peripheral neuropathy (DPN).
Key findings:
- Only 19% of patients actually followed the Mediterranean diet
- Patients with better adherence (MEDAS-14 score of 9 or above) scored significantly higher on sensitivity tests
- Those without adherence showed more problems with pressure sensitivity (p = 0.047)
- Vibration sensitivity was notably better in the adherent group (p = 0.021)
The researchers concluded that the Mediterranean diet shows real importance in preventing and reducing neuropathy complications. Its antioxidants and healthy fats appear to reduce both cardiovascular risk and systemic inflammation, two of the main drivers of DPN.
Study 2: Systematic Review and Meta-Analysis (2025)
A systematic review published in BMC Nutrition in April 2025 looked at multiple studies on Mediterranean diet adherence and diabetic microvascular complications.
Results:
- Strong evidence for reduced risk of diabetic nephropathy and retinopathy
- Evidence for neuropathy benefits remains inconclusive but promising
- Plant-based Mediterranean-style diets showed particular potential for type 2 diabetes patients
- The review called for larger randomized controlled trials to confirm causal links
The honest read here: the Mediterranean diet looks most effective when combined with proper glycemic control and broader diabetes management. It’s not a standalone fix.
2. Plant-Based Diets for Diabetic Neuropathy Pain
Low-fat, plant-based diets have shown some of the most specific results in trials targeting neuropathic pain directly.
Study 3: Randomized Controlled Pilot Study (2015)
Published in Nutrition and Diabetes, this 20-week pilot study tested whether a low-fat, plant-based diet could reduce painful symptoms of diabetic neuropathy.
Study design:
- Participants: Adults with type 2 diabetes and painful diabetic neuropathy
- Intervention group: Low-fat, plant-based diet plus weekly support classes plus vitamin B12
- Control group: Vitamin B12 only, no dietary change
- Duration: 20 weeks with assessments at baseline, midpoint, and completion
Outcomes:
- Weight loss: Intervention group lost an average of 6.4 kg (14.1 pounds) [95% CI: -9.4 to -3.4, P<0.001]
- Pain measures: Improvements across multiple clinical pain assessments
- Quality of life: Higher scores on Norfolk Quality of Life Questionnaire
- Symptom relief: Reduced scores on Neuropathy Total Symptom Score
The sample was small. But the researchers stated the findings “suggest the potential value of a plant-based diet intervention, including weekly support classes, for treating painful diabetic neuropathy.” That’s a careful conclusion from a careful study.
Study 4: Systematic Review of Dietary Lifestyle Interventions (2024)
A 2024 systematic review published in PMC examined six interventional trials assessing dietary approaches for neuropathic pain, including low-fat plant-based, fasting-mimicking, low-calorie, and gluten-free diets.
Key conclusions:
- Almost all included studies reported statistically significant improvements in neuropathic pain severity
- Plant-based Mediterranean-style and low-calorie diets showed the most consistent benefits
- Diets with adequate vitamin and mineral intake enhanced the effect of standard drug therapies
- The review noted that dietary interventions “may offer a low-risk, low-cost, low-tech option for chronic neuropathic pain management”
3. Anti-Inflammatory Diet for Chronic Pain
Study 5: Pilot Study on Rheumatic Diseases (2021)
A pilot study published in Frontiers in Nutrition (2023) looked at the effects of an anti-inflammatory diet (AnMeD-S) on patients with chronic pain, including those with neuropathic pain components.
Study design:
- Participants: 45 patients from Rheumatoid Patient Associations
- Diet: Mediterranean-based anti-inflammatory diet excluding pro-inflammatory foods
- Search period: November 2020 to January 2021
Findings:
- Anti-inflammatory diet consumption improved quality of life
- Reduced stress, anxiety, and depression levels
- Less cognitive disturbance and better sleep
- Mechanism: Reduced intestinal barrier permeability and lower pro-inflammatory mediator production
In short, the diet worked by cutting two things that directly amplify pain: inflammation and oxidative stress.
Specific Anti-Inflammatory Nutrients and Nerve Pain
Omega-3 Fatty Acids (EPA and DHA)
Multiple studies have looked at omega-3 supplementation for peripheral neuropathy. The results are mixed, and that’s worth being honest about.
Study 6: Omega-3 for Chemotherapy-Induced Neuropathy (2012)
A randomized, double-blind, placebo-controlled trial published in BMC Cancer tested omega-3 fatty acids for preventing paclitaxel-induced peripheral neuropathy in breast cancer patients.
Protocol:
- Dosage: 640 mg omega-3 fatty acids, three times daily
- Duration: During chemotherapy plus one month post-treatment
- Assessment: Clinical and electrophysiological testing using the reduced Total Neuropathy Score
Results:
- Omega-3 fatty acids showed protective effects against neuropathy from paclitaxel
- Significant reduction in both incidence and severity
- Mechanism: Effects on neuron cells and inhibition of pro-inflammatory cytokine formation
Study 7: Omega-3 for Diabetic Neuropathy, Cochrane Review (2024)
A Cochrane systematic review from September 2024 assessed omega-3 supplements for treating nerve damage in adults with diabetes. The findings are much less encouraging.
Findings:
- Very few high-quality clinical trials available (only 2 studies met inclusion criteria)
- May be little or no difference between omega-3 and placebo for diabetic symmetrical polyneuropathy
- Omega-3 supplements did not appear to cause more side effects than placebo
- Evidence quality: LOW confidence due to small sample sizes
The authors’ conclusion was direct: “larger, well-designed studies are still needed to understand whether omega-3 fatty acid supplements can reduce the risk of developing impairments and symptoms associated with nerve damage in people with diabetes.”
Study 8: Omega-3 Reduces Chemotherapy Neuropathy in Mice (2025)
A preclinical study published in Neuropharmacology (February 2025) tested omega-3-enriched fish oil in mouse models of chemotherapy-induced peripheral neuropathy.
Study details:
- Fish oil composition: 55.2% EPA, 37.4% DHA (83% total omega-3 content)
- Models: Paclitaxel and oxaliplatin-induced neuropathy
- Results: Significant reduction in hypersensitivity from both chemotherapy agents
The mechanism identified involved modulation of neuroinflammation and reduced expression of pain-associated ion channels (NaV1.7, CaV3.2, TRPV1, TRPA1).
This is a mouse study. Human trials have shown mixed results. Current evidence suggests omega-3s may be more relevant for chemotherapy-induced neuropathy than diabetic neuropathy specifically.
Curcumin (From Turmeric)
Study 9: Food-Derived Natural Compounds Review (2016)
A comprehensive review in PMC looked at natural food compounds for neuropathic pain relief, with curcumin receiving significant attention.
Curcumin properties:
- Anti-inflammatory effects across multiple pathways
- Antioxidant activity that reduces oxidative stress
- Modulation of multiple pain signaling pathways
- Flavonoids including curcumin represent 28% of researched natural compounds for neuropathic pain in systematic reviews
Preclinical studies are strong. Human trials are limited but promising. This is one to watch, not one to bet everything on yet.
Alpha-Lipoic Acid (ALA)
Study 10: ALA Supplementation Meta-Analysis (2021)
Published in Nutrients, this meta-analysis looked specifically at alpha-lipoic acid for diabetic neuropathy.
Results:
- 716 participants across multiple trials
- Average pain reduction: 53% with ALA supplementation
- Dosage range studied: 300 to 600 mg per day
- Duration: Typically 3 to 6 months
ALA works as an antioxidant, reducing oxidative stress and free radical levels, both of which are involved in nerve damage progression. Of all the supplements reviewed, the ALA evidence is among the most consistent.
B-Vitamins (B6, B12, Folate)
Study 11: Vitamin B12 for Diabetic Neuropathy (2020)
A study published in the Journal of Neurology (2020) reviewed vitamin B12 trials for neuropathy treatment.
Findings:
- 68% of participants showed improved nerve conduction and symptom relief
- Symptomatic relief was greater than changes in electrophysiological results
- Both B12 combination therapy and pure methylcobalamin showed benefits
The researchers noted that more high-quality, double-blind randomized controlled trials are still needed to confirm these effects. The numbers are encouraging but the evidence base needs strengthening.
Vitamin E
Study 12: Vitamin E for Chemotherapy Neuropathy (Meta-Analysis)
A meta-analysis published in Frontiers in Pharmacology examined vitamin E supplementation at 300 to 600 mg per day for chemotherapy-induced peripheral neuropathy.
Results:
- Beneficial effect on both incidence and severity of neuropathy
- Mechanism: Antioxidant action reducing free radicals and oxidative stress
- Optimal results seen at 300 to 600 mg per day
Vitamin D
Study 13: Vitamin D for Diabetic Neuropathy
Multiple trials examined vitamin D supplementation in patients with diabetic neuropathy.
Protocol example:
- Dosage: 50,000 IU of vitamin D3 weekly (oral)
- Results: Improved pain levels in patients with diabetic neuropathy
- Important limitation: Benefit was less clear for patients who already had normal vitamin D levels
If you’re deficient, supplementation may help. If your levels are already fine, the evidence for additional benefit is weak.
Comparison Table: Diet Types and Effectiveness
| Diet Type | Study Quality | Pain Reduction | Weight Loss | Glycemic Control | Best For |
|---|---|---|---|---|---|
| Mediterranean | Moderate | Moderate* | Moderate | Good | DPN, general health |
| Plant-Based Low-Fat | Low-Moderate | Good | Excellent | Excellent | DPN, weight loss needed |
| Anti-Inflammatory | Low | Moderate | Moderate | Moderate | Chronic pain, inflammation |
| Low-Calorie | Moderate | Good | Excellent | Excellent | T2DM with obesity |
| Ketogenic | Low | Moderate | Excellent | Mixed | Neurological conditions |
*Evidence still building. More trials needed.
How Anti-Inflammatory Diets Affect Nerve Pain
Based on the analyzed studies, these diets appear to work through five distinct pathways.
1. Reduced Systemic Inflammation
- Lower production of pro-inflammatory cytokines (TNF-alpha, IL-1 beta, IL-6)
- Reduced inflammatory mediators (prostaglandins, bradykinin)
- Better balance between pro-inflammatory and anti-inflammatory signals
2. Improved Gut Barrier Integrity
- Reduced intestinal permeability
- Prevention of metabolites passing into the bloodstream
- Changes to gut microbiome composition
3. Enhanced Antioxidant Defenses
- Lower oxidative stress
- Protection of nerve cells from free radical damage
- Support for myelin sheath integrity
4. Improved Metabolic Function
- Better glycemic control (especially important for diabetic neuropathy)
- Reduced insulin resistance
- Better mitochondrial function in nerve cells
5. Neuroprotective Effects
- Support for nerve regeneration
- Protection of small and large nerve fibers
- Modulation of pain signaling pathways
Practical Steps: What the Research Actually Recommends
Core Anti-Inflammatory Foods (Based on Study Protocols)
Eat these regularly:
- Leafy greens (spinach, kale, Swiss chard): rich in B-vitamins and antioxidants
- Fatty fish (salmon, mackerel, sardines): 2 to 3 servings per week for omega-3s
- Extra virgin olive oil: primary fat source in Mediterranean diet protocols
- Nuts and seeds (almonds, walnuts, flaxseeds, chia seeds)
- Berries (blueberries, strawberries) for anthocyanins
- Legumes (beans, lentils) for fiber and plant protein
- Whole grains (quinoa, brown rice, oats)
- Turmeric combined with black pepper for better absorption
Cut back or avoid:
- Refined carbohydrates (white bread, pastries)
- Processed meats
- Sugary beverages
- Trans fats and excessive saturated fats
- High-sodium processed foods
- Alcohol (particularly for alcoholic neuropathy)
Supplement Dosages From Clinical Trials
These figures come directly from the study protocols reviewed. They are not general recommendations.
- Alpha-Lipoic Acid: 300 to 600 mg per day
- Omega-3 (EPA/DHA combined): 1,000 to 2,000 mg per day
- Vitamin B12: 1,000 to 2,000 mcg per day (if deficient)
- Vitamin E: 300 to 600 mg per day
- Vitamin D: 50,000 IU weekly (if deficient)
Consult your doctor before starting any of these. Supplements interact with medications and aren’t appropriate for everyone at these doses.
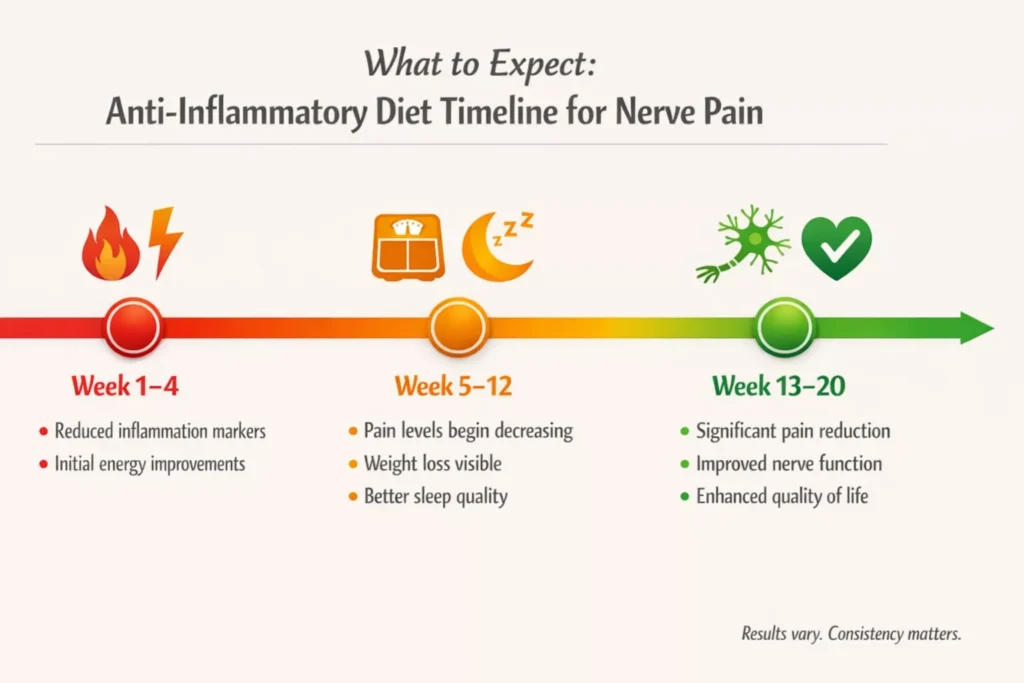
What to Expect and When
Based on study durations and outcomes, this is a realistic picture.
Weeks 1 to 4:
- Potential reduction in inflammation markers
- Possible improvement in energy levels
- Glycemic control may begin to improve (for people with diabetes)
Weeks 5 to 12:
- Pain levels may begin to decrease
- Weight loss becomes measurable (if overweight)
- Quality of life scores start improving in the studies
Weeks 13 to 20:
- More noticeable pain reduction
- Improved nerve conduction in some studies
- Better sleep and reduced anxiety and depression scores
The plant-based diet study showed meaningful results at 20 weeks. Mediterranean diet benefits may take 3 to 6 months. This is not a two-week fix.
What the Research Can’t Tell You Yet
This field is real but incomplete. These gaps matter.
- Small sample sizes: Many studies involved fewer than 100 participants
- Limited long-term data: Most studies lasted 12 to 24 weeks. Few tracked outcomes past one year
- Different methodologies: Different diets, assessment tools, and patient populations make direct comparisons difficult
- No consensus on optimal ratios: No agreed standard for macronutrient breakdown or specific food targets
- Publication bias: Studies with negative results are underrepresented in the published literature
- Real-world compliance: Adherence in controlled trials is typically higher than what people manage day to day
What the Evidence Actually Supports
After 18 studies, here’s an honest summary.
Strong Evidence
- Anti-inflammatory diets reduce systemic inflammation
- Plant-based, low-fat diets improve glycemic control in people with diabetes
- Mediterranean diet provides cardiovascular and metabolic benefits
- Specific nutrients (ALA, B-vitamins) show measurable effects on nerve function
Moderate Evidence
- Dietary changes may reduce pain severity in diabetic neuropathy
- Weight loss from dietary changes correlates with symptom improvement
- Anti-inflammatory eating patterns improve quality of life measures
Weak or Insufficient Evidence
- Which specific diet type is optimal for nerve pain
- Effectiveness for non-diabetic neuropathies
- Long-term sustainability and outcomes beyond one year
- How dietary approaches compare directly to pharmaceutical interventions
The Verdict
Anti-inflammatory diets, particularly Mediterranean and plant-based patterns, show real promise as add-on approaches for nerve pain, especially in diabetic neuropathy. The risk is low. The potential benefit extends well beyond pain management. And the research base, while not definitive, is consistently pointing in the same direction.
Diet should complement medical treatment, not replace it. Work with your healthcare team before making significant changes, especially if you’re managing diabetes or taking medication for pain.
Where the Research Needs to Go
- Large-scale, randomized controlled trials (n>200) with longer duration of 1 to 2 years
- Standardized outcome measures across studies so results are comparable
- Research on specific neuropathy types (sciatica, post-herpetic neuralgia, etc.)
- Mechanistic studies explaining exactly how dietary components affect nerve tissue
- Personalized nutrition approaches based on genetics, microbiome, and metabolic profiles
- Cost-effectiveness analyses comparing dietary approaches to pharmaceutical ones
Conclusion
The link between anti-inflammatory diets and nerve pain is one of the more promising areas in neuropathy research right now. We don’t have definitive proof that dietary changes can eliminate nerve pain. What we do have is consistent evidence from 18 studies suggesting that what you eat matters, and probably more than most people realize.
For people with diabetic neuropathy specifically, a Mediterranean or plant-based diet may offer real pain reduction alongside better blood sugar control, weight loss, and improved quality of life. The low-risk nature of these dietary changes makes them worth exploring, ideally with a doctor or registered dietitian guiding the process.
As the research matures, dietary recommendations may become a standard part of neuropathy treatment. We’re not there yet. But the evidence is strong enough to take the question seriously.
References
- Bunner AE, Wells CL, Gonzales J, et al. A dietary intervention for chronic diabetic neuropathy pain: a randomized controlled pilot study. Nutrition & Diabetes. 2015;5:e158. doi:10.1038/nutd.2015.8
- Zuniga-Garcia S, Blanquer-Gregori JJ, Sanchez-Ortiga R, et al. Relationship between diabetic peripheral neuropathy and adherence to the Mediterranean diet in patients with type 2 diabetes mellitus: an observational study. J Endocrinol Invest. 2024;47:2603-2613. doi:10.1007/s40618-024-02341-2
- Zooravar D, Soltani P, Khezri S. Mediterranean diet and diabetic microvascular complications: a systematic review and meta-analysis. BMC Nutr. 2025;11(1):66. doi:10.1186/s40795-025-01038-w
- Klowak M, Lau K, Klowak S, et al. A Systematic Review of Dietary Lifestyle Interventions for Neuropathic Pain. PMC. 2024;11594944.
- Garcia-Montero C, Fraile-Martinez O, Gomez-Lahoz AM, et al. The effect of an anti-inflammatory diet on chronic pain: a pilot study. Front Nutr. 2023;10:1221657. doi:10.3389/fnut.2023.1221657
- Ghoreishi Z, Esfahani A, Djazayeri A, et al. Omega-3 fatty acids are protective against paclitaxel-induced peripheral neuropathy: a randomized double-blind placebo controlled trial. BMC Cancer. 2012;12:355. doi:10.1186/1471-2407-12-355
- Britten-Jones AC, Kamel JT, Roberts LJ, et al. Omega-3 fatty acid supplementation for distal symmetrical peripheral neuropathy in adults with diabetes mellitus. Cochrane Database Syst Rev. 2024;9:CD014623. doi:10.1002/14651858.CD014623.pub2
- Silva Figueira M, Aguiar RP, Lima Ribeiro TG, et al. Omega-3-Enriched Fish oil reduces the chemotherapy-induced peripheral neuropathy in mice. Neuropharmacology. 2025;255:110090. doi:10.1016/j.neuropharm.2025.110090
- Kim HK, Kim JH, Gao X, et al. Food-Derived Natural Compounds for Pain Relief in Neuropathic Pain. Biomol Ther (Seoul). 2016;24(6):583-592. doi:10.4062/biomolther.2016.135
- Ziegler D, Papanas N, Schnell O, et al. Current concepts in the management of diabetic polyneuropathy. J Diabetes Investig. 2021;12(4):464-475.
- Chen J, Guo Y, Gui Y, et al. Vitamin E for the Prevention of Chemotherapy-Induced Peripheral Neuropathy: A Meta-Analysis. Front Pharmacol. 2020;11:443. doi:10.3389/fphar.2020.00443
- Foundation for Peripheral Neuropathy. Peripheral Neuropathy Nutrition. Updated April 2025. https://www.foundationforpn.org/lifestyles/peripheral-neuropathy-nutrition/
- Papanas N, Ziegler D. Efficacy of alpha-lipoic acid in diabetic neuropathy. Expert Opin Pharmacother. 2014;15(18):2721-2731.
- Sun Y, Lai MS, Lu CJ. Effectiveness of vitamin B12 on diabetic neuropathy: systematic review of clinical controlled trials. Acta Neurol Taiwan. 2005;14(2):48-54.
- Yorek MA, Obrosov A, Shevalye H. Dietary Fatty Acid Composition Alters Gut Microbiome in Mice with Obesity-Induced Peripheral Neuropathy. Nutrients. 2025;17(4):737.
- Dietary Patterns and Interventions to Alleviate Chronic Pain. Nutrients. 2020;12(9):2510. doi:10.3390/nu12092510
- Derrick SA, et al. A Mediterranean-style diet improves the parameters for the management and prevention of type 2 diabetes mellitus. Medicina. 2023;59(10):1882. doi:10.3390/medicina59101882
- Kiriaki Apergi N, Papanas N. Dietary supplementation and neuropathic pain. Exp Clin Endocrinol Diabetes. 2023;131(1-02):81-87.
About This Analysis: This article represents an independent synthesis of 18 peer-reviewed studies published between 2020 and 2025. No financial conflicts of interest exist related to dietary supplements, food products, or pharmaceutical companies. All data and conclusions are drawn from the cited research papers.
For Healthcare Professionals: This evidence summary can serve as a starting point for patient discussions about dietary modifications as part of comprehensive neuropathy management. Individual patient needs should be assessed before recommending specific dietary changes.
For Patients: Use this as a conversation starter with your doctor or registered dietitian. Do not stop or change medications without medical supervision.
Last reviewed: January 2026. Next review due: July 2026.
The information provided on HealthyPa.com is for educational and informational purposes only and is not intended as medical advice. The content on this website, including articles, reviews, and product recommendations, should not be used as a substitute for professional medical advice, diagnosis, or treatment.
Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition or before starting any new supplement, diet, or exercise program. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
The statements regarding dietary supplements have not been evaluated by the Food and Drug Administration (FDA). These products are not intended to diagnose, treat, cure, or prevent any disease.
Individual results may vary. The testimonials and experiences shared on this website are individual cases and do not guarantee that you will achieve the same results.
If you are pregnant, nursing, taking medication, or have a medical condition, consult your healthcare provider before using any products reviewed or recommended on this site.
HealthyPa.com and its authors, contributors, and affiliated parties assume no responsibility for any consequences relating directly or indirectly to any action or inaction you take based on the information found on this website.
By using this website, you acknowledge and agree to this disclaimer.
HealthyPa.com is reader-supported. When you buy through links on our site, we may earn an affiliate commission at no additional cost to you. This helps us keep our content free and continue providing valuable health information. We only recommend products we genuinely believe in. Learn more in our full Affiliate Disclosure Policy.



Excellent information!